It’s estimated that approximately 82.1 million adults in the United States spend an estimated $28.6 billion on gym memberships each year! Now combine that staggering number with the estimated $50 billion dollars plus spent annually on back pain related issues. Even with the general fitness craze we have seen over the past years, low back pain (LBP) remains one of the most prevalent medical conditions treated in the United States and throughout the western world. It affects nearly 80% of the U.S. population at one time or another. It’s one of the top reasons for physician visits and one of the most common reasons for missed work days.
With so many active individuals and crazy fitness trends you would think that all of this exercise would actually help reduce low back pain, right? Wrong…It turns out that not all exercise (and especially, not all “core” exercise) is created equally.

It’s time to address how to safely self-treat your low back pain through movement and exercise as well as some helpful methods for a speedy recovery. (Not to mention, possibly saving you time and money by avoiding a physician visits for pain you can manage safely and independently with a little instruction.)
To safely self-treat your low back pain, first take a moment to assess your symptoms and pain level. What led to your pain and/or injury? Did the pain come on suddenly or slowly? Evaluate the severity of the injury. If you’re experiencing any of the following, please seek immediate medical attention:
- Loss of bowel/bladder function.
- Uncontrollable pain. The pain is so severe you cannot function or move.
- You are losing muscle function or control. The muscles in the legs will no longer work. (This is different than pain preventing the muscle from working.) This sensation of paralysis occurs when the muscles will not actually function.
- Significant loss of sensation in the leg or groin area. This is not a tingling sensation, but an actual loss of sensation. For example, you cannot feel the toilet paper when you wipe after using the toilet.
- Onset of pain without any known mechanism for the injury. (Thoroughly consider your activity. Many times, a slow onset of pain begins several hours after performing an activity.)
Fortunately, most LBP is mechanical–meaning it is from a physical or structural cause and isn’t related to conditions such as cancer or infections. Most LBP will have a directional preference for extension. A majority of injuries occur when performing a forward biased (flexed movement) like chronic slouching or a spinal flexion biased movement. For discussion purposes, I will be addressing an extension biased program.
With mechanically driven low back pain, you should be able to alter and change your LBP within a short period of time. First, establish a directional preference by identifying a pattern to the pain. Does the pain get worse when you bend over or does it improve? What happens when you repeat this movement?
Determine how your pain responds. If it spreads away from the spine and down into the leg, beware that you are moving in the wrong direction. Stop that particular movement, and instead try flexion biased movements. In my experience, most episodes of LBP tend to respond better to extension biased movements. If flexion or extension doesn’t help or change the pain in any way, then you may need assistance from a medical provider.
The rule of thumb for movement: If the pain worsens by spreading peripherally down the buttock and into the leg and/or foot, then the condition is worsening. We must stop that activity. If the pain centralizes and returns back toward the spine (even if the pain worsens slightly), then keep moving as the condition is actually improving.
Although most LBP isn’t considered serious, the pain tends to re-occur. One major reason for this is that the deep stabilizing muscles known as the multifidus muscles reflexively shrink, weaken, and lose function. Without proper rehabilitation, the muscles will not fully recover. This increases the risk of future episodes because the spine no longer has the ability to stabilize itself normally. Not all “core” work is created equally, so the strength of these muscles needs to be addressed.
How to Safely Self-Treat Low Back Pain:
Perform Press-ups
Once you have injured your back, immediately start press-ups. Perform this exercise with high repetitions and frequently throughout the day as long as the pain does not periperalize down the buttock and into the leg and/or foot. Lie on your stomach and perform 10-20 press-ups. Move slow and easy, but work your way up to full motion multiple times a day.

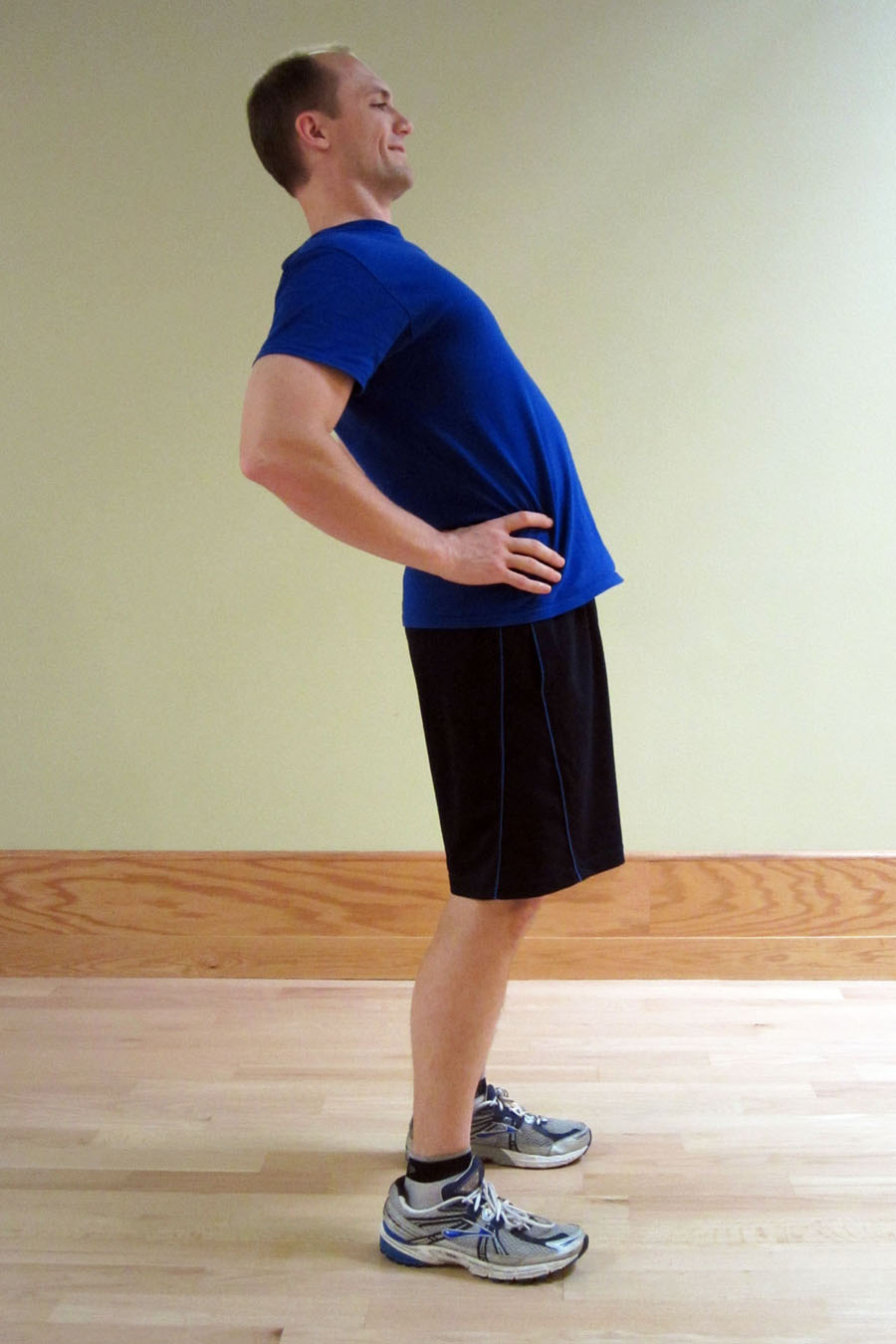
Perform Standing Back Extensions
After sitting, stand up and perform standing back extensions. Ideally, perform this exercise at least 10 repetitions each time you stand.
Activate the Multifidus
Start exercises to activate the multifidus muscles as soon as possible. Think spine extensor muscle activation. Again, perform this exercise frequently during the day after the initial injury. These Lumbar Extensor Exercises are designed to progressively activate the multifidus muscles (with the final exercise being the most challenging). Once the pain subsides and muscle function improves, more advanced lumbar extension strengthening and stabilizing exercises should be performed to decrease your risk of re-current low back pain.
Don’t Sit
Walking is critical to your recovery! It’s the number one way your spine receives nutrients and disposes of metabolic waste products. Walk frequently, and try to avoid any prolonged sitting.
If you Sit, Use Good Posture
Use a McKenzie Lumbar Roll to help insure a good lumbar curve. If you can’t sit comfortably, listen to your body and don’t sit! Be sure to stand up and walk every 20-30 minutes. Stand with good posture as well.
Stretch the Muscles of the Legs and Pelvis
Hip flexor and hamstring stretches can help to reduce muscle spasms and tightness throughout pelvis area when performed daily. Stretch for at least 30 seconds at a time, 2-3 times each session.

Be as Active as You Can
Don’t stop moving, but avoid exercises that make your back hurt more. Typically, this includes flexion biased movements like sit ups. It’s important that you remain as active as you can. You may need to taper down certain activities that you know will increase your pain. This typically would be activities involving heavy loading of the spine such as squats with weight, deadlifts, and other activities that may cause forward flexion (particularly under a load).
As you are able to, continue to work on cardiovascular conditioning and core muscle activation (particularly, the lumbar extension exercises). Basically stay as active as you can, even lifting weights if you are able. Just remember the concept of peripheralization and centralization. If your pain progresses from the area of the injury into your leg, then you need to stop that activity. If the pain remains constant or is progressing out of the leg, then continue with the activity as you are helping the body to heal.
Developing adequate strength in the lumbar extensor muscles and core musculature is the primary way to prevent initial episodes and to prevent reoccurring episodes of LBP. Research clearly indicates that the right targeted exercises are the most effective way to manage LBP.
If you’re not sure how to effectively and safely exercise your back or if you’re already experiencing low back pain, be sure to check out my Treating Low Back Pain (LBP) during Exercise and Athletics Book and Video Package. USE DISCOUNT CODE LBP AT CHECKOUT FOR 15% OFF!
For the approximate price of just one co-pay to see a doctor, you will receive my easy to read book with step-by-step instructions and a complete video package designed to help you prevent and self-treat reoccurring low back pain episodes.
Want to peek inside the video content? Watch now as I describe what really the “core” is and why it matters.
If you have a question that you would like featured in an upcoming video or blog post, please comment below or submit your question to contact@thePhysicalTherapyAdvisor.com. In case you haven’t already, be sure to subscribe to my e-mail list and YouTube channel as well as join our community on Facebook by liking The Physical Therapy Advisor!